What is Osseointegration?
Osseointegration (also known as Direct Skeletal Fixation -DSK) involves inserting a prosthetic implant into the residual bone of an amputee to which an external prosthesis can attach directly. This removes the need for a traditional socket-mounted prosthesis.
This surgical solution uses cutting-edge technology to enhance the mobility and quality of life of amputees.
What are the Benefits of Osseointegration?
Why choose Osseointegration? There are several benefits to amputees of Osseointegration compared to traditional prosthetics:
No More Sockets
No more sweating, rubbing, bruising, chafing and discomfort caused by your socket.
Easy Attachment
One screw to attach and remove your prosthesis is completed in seconds
Improve Mobility & Gait
Increased muscle use and control allow a more natural gait with increased range of motion.
Direct Mechanical Control
You’ll have full control of your limb with direct mechanics and improved osseoperception.
Fast Rehabilitation
An accelerated surgical and rehabilitation program reduces the overall recovery time to 4-6 weeks.
Lower Cost
Regular socket re-fittings are no longer required which can represent significant cost savings.
Is Osseointegration for Amputees Widely Used?
Over 2,000 patients have Osseointegration surgeries. Osseointegration Group has over 1,200 successful osseointegration cases worldwide. This makes Osseointegration Group the most experienced team in the world.
Find out how Osseointegration has helps these patients in the UK:
Who is Osseointegration Group?

Prof. Munjed Al-Muderis is a major figure in the field of osseointegration surgery, improving the implant and the surgical technique while re-designing the first phase of the rehabilitation for patients undergoing osseointegration.
He is credited with taking a surgical technique that was considered experimental and making it routine.
In 2010 he founded Osseointegration International to make this application available worldwide by partnering with a team of expert surgeons who could be fully trained in the surgical procedure. By constantly networking, they can improve surgical techniques, rehabilitation processes, and patient care.
Prof. Al-Muderis performs operations in Europe from a number of centres. For more information on Prof. Al-Muderis’s availability, please enquire.

Dorset Orthopaedic’s experienced inter-disciplinary team of clinicians, comprising prosthetists, orthotists and physiotherapists, use a holistic approach to provide the most up to date components, alongside specialist training in order to maximise patients mobility, independence and overall quality of life.

Why Choose Osseointegration Group in the UK?
Unparalleled Experience
With 12 global centres, OI has performed over 1,200 operations. This makes us the most experienced team in the world.
The UK team has decades of combined experience and hundreds of patient success stories transforming amputees’ quality of life.
Their unique background in reconstructive plastic surgery means they look at the whole picture and provide you with holistic care that makes a difference.

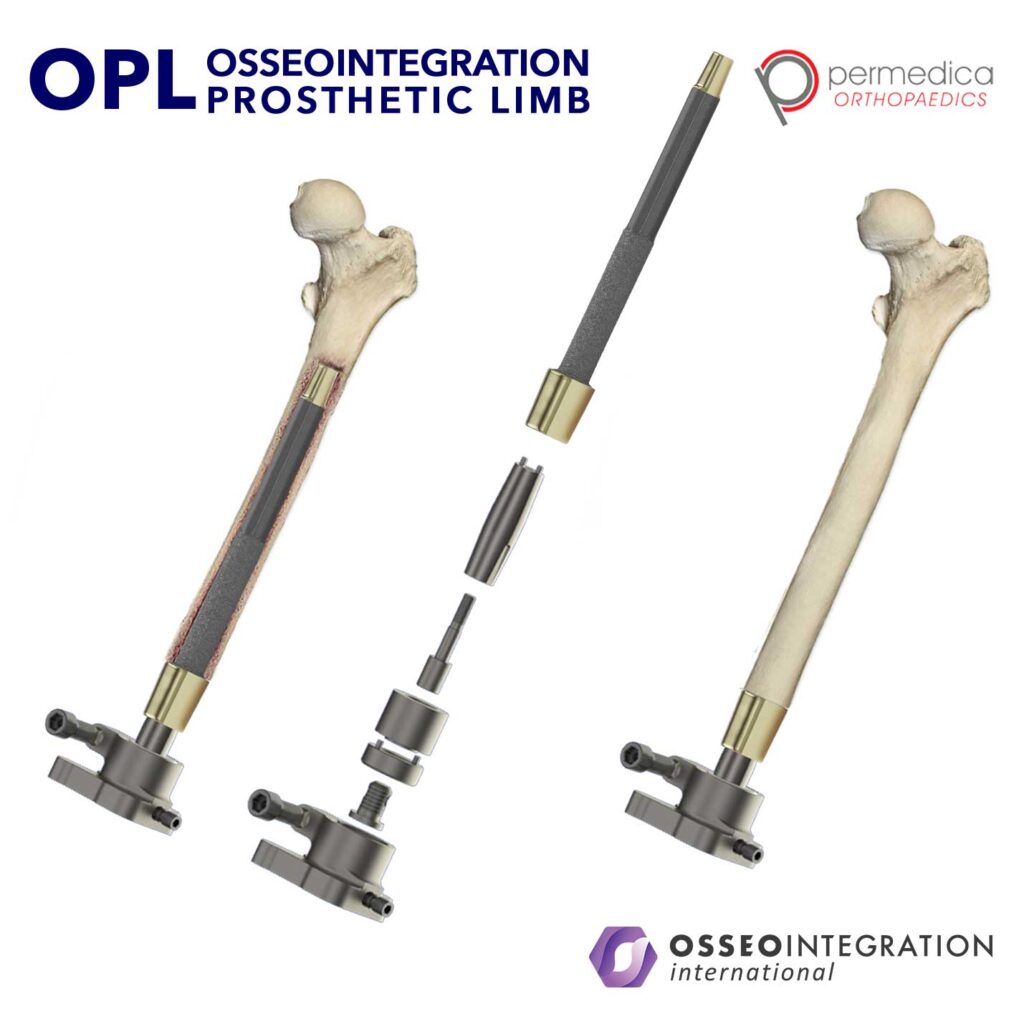
Optimised Prosthesis
Designed by Prof. Al Muderis, and manufactured by Permedica, the prosthesis has a unique press-fit design that takes the load back directly to the bone and the associated muscles.
The prosthesis is implanted directly into the bone and encourages bone growth. Once integrated, it allows for a simple, quick, and safe connection between the residual limb and the lower prosthesis.
One Procedure
In most cases, unlike other osseointegration procedures, just one surgical procedure is required. This means less time in the operating theatre and quicker rehabilitation.
Recent studies have shown there are fewer complications with a one-stage approach (https://boneandjoint.org.uk/Article/10.1302/2633-1462.47.BJO-2022-0117.R1)
In very complex cases where bone lengthening or alignment correction is required, multiple procedures may be required.

The World's Largest Osseointegration Peer Support Group
It’s no surprise that the team who has completed the most osseointegration surgeries also has the largest osseointegration support group.
Over 3,200 people comprising amputees and their families make up the Osseointegration Peer Support Group.
You will be in good company.
Osseointegration Patient Stories
There are hundreds of satisfied osseointegration patients who have benefited from the significant and unparalleled advantages compared to a traditional socket prosthesis. Here are just a few from around the world:
What to Expect From the Osseointegration Process
While every patient is unique to us, here is a snapshot of the typical process.
Pre-Surgery
A multidisciplinary team (MDT) will follow you throughout the entire first phase of the process. This is crucial for the success of the surgery.
Years of experience have enabled Osseointegration Group of Australia to develop a process that guarantees each patient is appropriately evaluated to verify eligibility.
Surgery
Surgery for osseointegration is usually performed under general anaesthesia.
First, the site is prepared for the implant.
Then the implant is carefully fitted.
Finally the procedure is completed by creating a circular opening (stoma) in the skin flap, allowing the tip of the implant to come through the skin.
Rehabillitation
Rehab is performed in 3 stages:
(Weeks 1-2): Initial loading until the target loading weight (50kg) or half the patient’s body weight is achieved.
(Weeks 3-6): Fitting of a light training prosthesis and start of gait training exercises.
(Weeks 7-14): Fitting of the definitive prosthesis, continuation of gait training exercises and mobilisation with crutches.
How Much Does Osseointegration Cost in the UK?
Osseointegration is major surgery and, by extension, the costs surrounding pre-surgery, surgery, and rehabilitation reflect that.
Costs vary greatly based on the particular situation and needs of each patient.
Every amputation is unique in:
- which limb is amputated,
- the level of amputation,
- the cause of amputation,
- the time since amputation,
- the individual’s bone quality,
- the amount of muscle and soft tissue coverage, and
- the integrity of the skin surrounding the residual stump.
As a result, these factors are all taken into consideration when planning what options are available and therefore each surgery plan and cost is prescribed individually to each patient.
Is Osseointegration available on the NHS?
Osseointegration is currently not funded by the NHS.
Will insurance pay for osseointegration?
Can I self-pay for osseointegration?
Yes.
Many osseointegration patients self-fund the procedure and rehabilitation.
Get in touch and we will organise a personalised quote for you based on your individual circumstances.
Osseointegration FAQs
All amputees are potential candidates for osseointegration. However, certain conditions such as age, smoking, ongoing chemotherapy, irradiated bone, ongoing infections, pregnancy, and psychological instability are regarded as additional risk factors to this procedure. Patients with diabetes and peripheral vascular disease are still eligible for consideration but will require extra precautions during the evaluation
- Above knee amputation
- Below knee amputation
- Above elbow amputation
- Below elbow amputation
- Digital/Finger amputation
No case is too challenging, the team is experienced in dealing with extremely complex cases.
Swimming in a pool, especially salt water or the sea, is highly recommended, as it helps to maintain stoma health. However, patients should minimize swimming in public pools, particularly those that are at risk of children defecating or urinating inside. Patients who swim in a public pool should ensure that the stoma is well rinsed when leaving the pool. Taking a bath with bathing salts is recommended from time to time, as this helps to treat muscle pain and prevent the accumulation of debris.
For the first 12 months following osseointegration surgery, patients are strongly advised against high impact activities such as running, or any activities that may result in a fall. Due to the affected limb being under-used prior to surgery, a period of at least 12 months is required for the development of bone strength to a level suitable for impact activities. Premature overloading of the bone will result in a greater risk of femoral neck fractures and other injuries. The patient is required to consult the principle surgeon before commencing any activities which may increase the risk of injury.
A stoma is a permanent opening into your body, a small amount of leakage daily of clear body fluid from the stoma in normal. Daily washing of the stoma in the shower using an antibacterial soap and a soft brush if required may be all that is required. Swimming in salt water or using Epsom Salt’s in a bath can be beneficial. Hype granulation is a common condition of the skin of the Stoma, it looks like hard bumpy or granular skin and forms beyond the surface of the stoma opening. If it causes pain it can be removed by your GP using Silver Nitrate to cauterise the growth.
Clear mucous secretions from the stoma site are normal, and can increase with higher activity levels and alcohol consumption. However, milky discharge accompanied by pain is often a sign of infection. Certain people can also manifest lack of secretion and dry crust formation at the stoma site, which needs to be cleaned regularly to prevent infection
Normally there should be no pain from the residual bone, if pain occurs it could be due to a skin infection around the stoma. In this case, a swab taken by your GP for testing and a course of antibiotics if required normally resolves the issue. Deeper pain could also be due to a neuroma which is often described as a pinched nerve or burning sensation, it is actually a benign growth of nerve tissue and may require surgery to remove. Deep infection that necessitates removal of the stem implant is very rare but if required can be treated and a new stem re inserted.
Please discuss any phantom or neuroma pain you may be experiencing with the surgeons during the planning stage before your Osseointegration as a procedure called Targeted Muscule Reinnervation (TMR) can be performed at the same time which has demonstrated promising results in reducing pain.
There are only a small fraction of cases reported worldwide that required replacement or removal of the implant. It is quite rare that the procedure results in the loss of the rest of the residual limb. If the surgery does not work for some reason, the patient can always choose to return to a socket prosthesis. It’s important to note that any surgery could potentially result in devastating complications including death. Osseointegration carries similar risk as any medium complexity orthopedic surgery.
Patients who suffer from this pain have had, in many occasions, significant relief from this condition. This is due to a combination of pharmaceutical and surgical intervention.
Surgery costs vary greatly based on the particular situation and needs of each patient.
Every amputation is unique in what limb is amputated, the level of amputation, the cause of amputation, the time since amputation, the individual’s bone quality, the amount of muscle and soft tissue coverage and the integrity of the skin surrounding the residual stump. As a result, these factors are all taken into consideration when planning what options are available and therefore each surgery plan and costing is prescribed individually to each patient.
Next Steps...
Imagine a life without a socket. A leg that is not cumbersome, that didn’t cause rubbing.
A fit that is so close to normality it is changing lives for the better.




